LASIK Side Effects And Complications
LASIK is a popular solution to vision problems. Like any other surgery, there are potential LASIK side effects and complications.
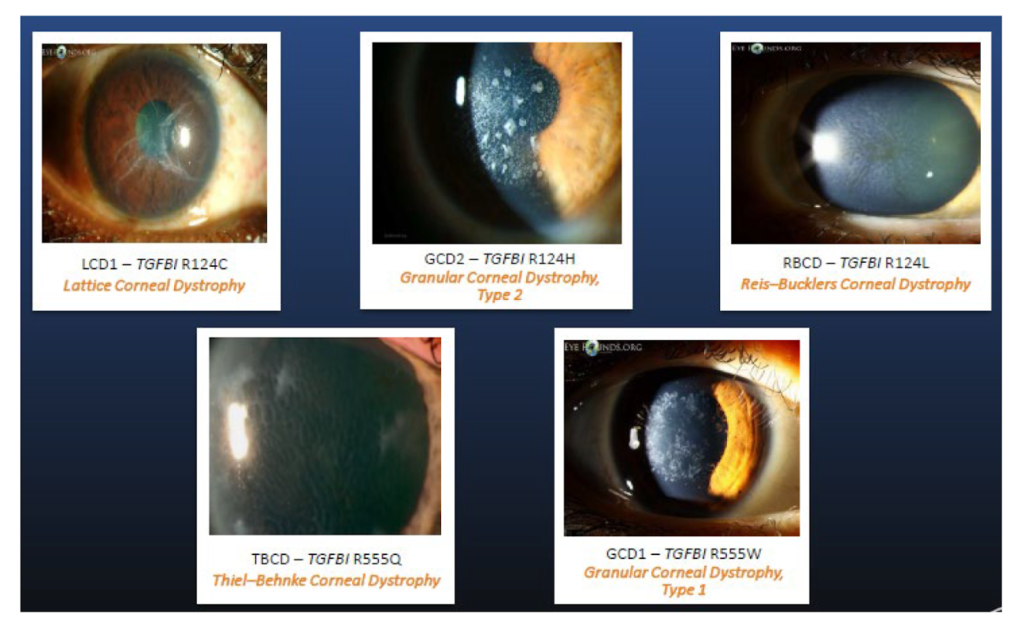
Corneal Dystrophy is a group of hereditary diseases in which a specific grey-white protein accumulates in the cornea during recovery after a physical wound, caused by abnormal operation of the repair mechanism due to a gene mutation.
South Korea
China
USA
It is important to know about corneal dystrophy because it is a genetic disease that still has no cure. As there is no way to reverse the disease once it has progressed, it is important to delay the onset of the disease as much as possible.
Corneal dystrophy is basically a genetic disorder. Even if no family member or relative has the corneal dystrophy mutation, the mutation can be passed on to the next generation.
Ultraviolet light or physical injury of the cornea may exacerbate the symptoms or impact the progression of corneal dystrophy.
An ophthalmologist’s instrumental examination may confirm corneal dystrophy, but it may be difficult to accurately identify a person with minimal or no symptoms. Therefore, it is recommended to accurately identify the disease using genetic testing.
Most patients with corneal dystrophy in the early stages have a clear cornea, and even if it is developed, it may be difficult to obtain accurate results because the degree of expression varies due to differences in individual living environments and long-term wearing of lenses.
When genetic testing is used, even in the case of patients who are difficult to judge with an ophthalmological equipment test, patients can be selected with accurate judgment criteria. In addition, many textbooks and literature stipulate that it is advisable to contraindicate refractive surgery such as LASIK and LASIK for those who have a mutant gene associated with corneal dystrophy.
Corneal transplantation is a surgical procedure for corneal dystrophy. Vision can be temporarily secured by cutting the cornea, but it soon recurs and worsens.
Although corneal dystrophy can be temporarily treated through a therapeutic laser keratectomy, Phototherapeutic Keratectomy or PTK that partially removes the opaque corneal layer, the corneal dystrophy recurs over time, resulting in more severe opacity. That is why it is important to slow the onset and progression of the disease as much as possible.
There is still no cure for corneal dystrophy. Once diagnosed with corneal dystrophy, as a preventive measure, the best way to prevent physical damage to the cornea is to correct your lifestyle and monitor it regularly.
1. It is recommended to avoid refractive surgery such as LASIK.
2. In order to slow the progression of the disease as much as possible, avoid external stimuli such as UV rays. For outdoor activities, it is recommended to wear protective glasses with UV protection and a wide-brimmed hat.
3. Always take extra care of the eyes and avoid poking the eyes during strenuous exercise and everyday life.
4 Use artificial tears regularly.
If you have any queries or in need of assistance or advice regarding corneal dystrophy, send us a message by clicking the button below.

Related Articles To Corneal Dystrophy
LASIK is a popular solution to vision problems. Like any other surgery, there are potential LASIK side effects and complications.
Looking to get LASIK eye surgery? Before you do, it's important to be aware of the potential risks involved. This.
In this article, we delve into LASIK - what it is, how it works, the risks involved, and what to.